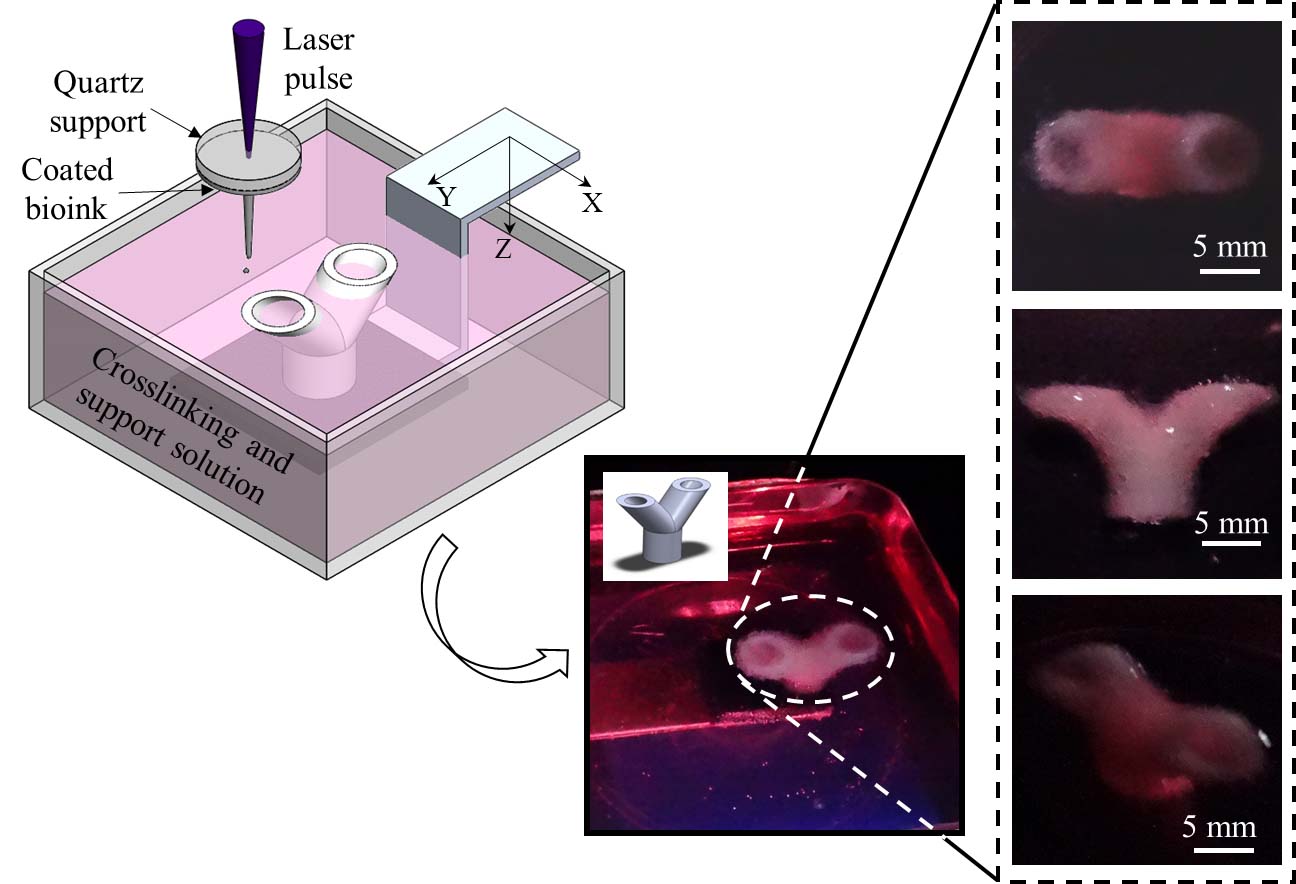
Tissue-engineering techniques such as bioprinting could one day be used to create biological tissues for transplantation. Professor Yong Huang’s lab and their Tulane University collaborator have successfully demonstrated the feasibility of laser printing straight and Y-shaped tubes with and without living cells. Dr. Yong Huang, a BME affiliate, is a professor in the department of mechanical and aerospace engineering at the University of Florida.
The demand for organ transplantation has rapidly increased all over the world, which has far exceeded the availability of organ donors, resulting is a severe organ shortage crisis. The ultimate goal of tissue engineering and regenerative medicine is to design and fabricate functional human tissues and organs suitable for the regeneration, repair, and/or replacement of damaged or injured human organs. In recent years, organ printing, among different tissue engineering innovations, is a layer-by-layer additive fabrication approach for making three-dimensional (3D) tissue and organ constructs using cellular spheroids or bioinks as building blocks.
Bioprinting-based organ printing provides a promising solution to the problem of organ donor shortage. While some major challenges are still in place, such as endothelialization and vascularization, there is a critical need to create technologies for the fabrication of hollow 3D vascular constructs for use as the first step in organ printing.
“Due to its potential in the freeform fabrication of 3D structures, I think that 3D bioprinting will eventually enable the printing of entire organs, bringing significant societal impacts,” said Yong Huang. In particular, Huang’s lab first demonstrated the feasibility of 3D laser bioprinting, which is more versatile in drop-on-demand printing highly viscous bioinks. Since it is an orifice-free technology, it has no concern of nozzle clogging as during inkjet bioprinting.
Next, Huang and colleagues plan to focus on printing 3D heterogeneous multicellular constructs, modelling of printing-induced cell injury, post-printing tissue fusion and maturation and clinical testing.